A Day with the Mobile Outreach Clinic

A Day with the Mobile Outreach Clinic
March 11, 2020 - Outreach Clinic in Kambulu, Kasungu, Malawi
7:30am
Leave Orant Charities Africa Campus
The team is a bit sleepy, but in high spirits. We climb into the ambulance, find our preferred seats, and prepare for the long drive ahead. Kambulu is one of the most distant villages that Orant’s outreach clinics visits. Though hard to reach, Kambulu is a necessary stop- the more remote the village, the less likely it is that the inhabitants will have regular access to healthcare. Our visit during the height of the malaria season in Malawi will no doubt save many lives.

9:35am
Arrival in Kambulu and Setup
The ride was long and bumpy (as always), but music helped pass the time. Happy, the driver and a patient care attendant backs the medical trailer into its usual place and the team begins unloading. There are already hundreds of people waiting to be seen. We make short work of unloading six crates, five tables, and seven chairs. The trailer itself acts as the mobile pharmacy. Upile, our star Pharmacy Assistant, has organized the trailer carefully and efficiently and will later distribute medicine from the inside.
There are six stations that make up our outreach clinics. These are Triage, Lab, Clinicians, Injection Room, Pharmacy, and Cashier.
9:45am
Triage
Our first stop is Triage. At Triage, clinicians take all patients’ temperatures, adult patients’ blood pressures, and children’s weights. Patients are sometimes visibly ill, they skip the line, fast track to see the clinician, and get tested immediately for malaria.
We set up the table, our battery-powered blood pressure machines, and scales, and begin seeing the patients that the village leaders have organized into a neat line. While Happy weighs the children, Peter is hard at work taking temperatures and checking blood pressure. Thomas, the nurse, also helps out when needed.
The patients give us their health passport. We record their vitals and send them to our clinicians. Our clinicians will give a diagnosis and a referral to the lab for testing, most often for malaria.
After a while, it begins to rain. We carry our table and scales to the cover of a large tree nearby. Most of the other stations were already inside local buildings or under trees, but the Lab has a lot of tests to pack up, so we run over there to help.
By 11:40, all the patients in line have been seen by Triage and have moved on to the other stations. Those working at Triage move on to help speed up the processes at the Lab, Pharmacy, and Cashier.

11:45am
Lab
At the Lab, we run tests on the patients to confirm the clinician’s suspicion of a disease or other problem. Memory, our hardworking Lab Assistant, is assisted by a local member of the health committee to prepare the hundreds of malaria tests that will be administered. More than 90% of the 2500+ tests we do in a month are malaria tests.Today is no different. Some patients, most often children, have severe malaria and must be rushed to the Injection Room to be treated. All those tested for malaria, young and old, will be added to the Malaria Register which allows the government and Orant to track the prevalence of malaria in each area.
As the Lab starts slowing down, we have already tested nearly 400 people for malaria and about 300 of them are positive.
12:45pm
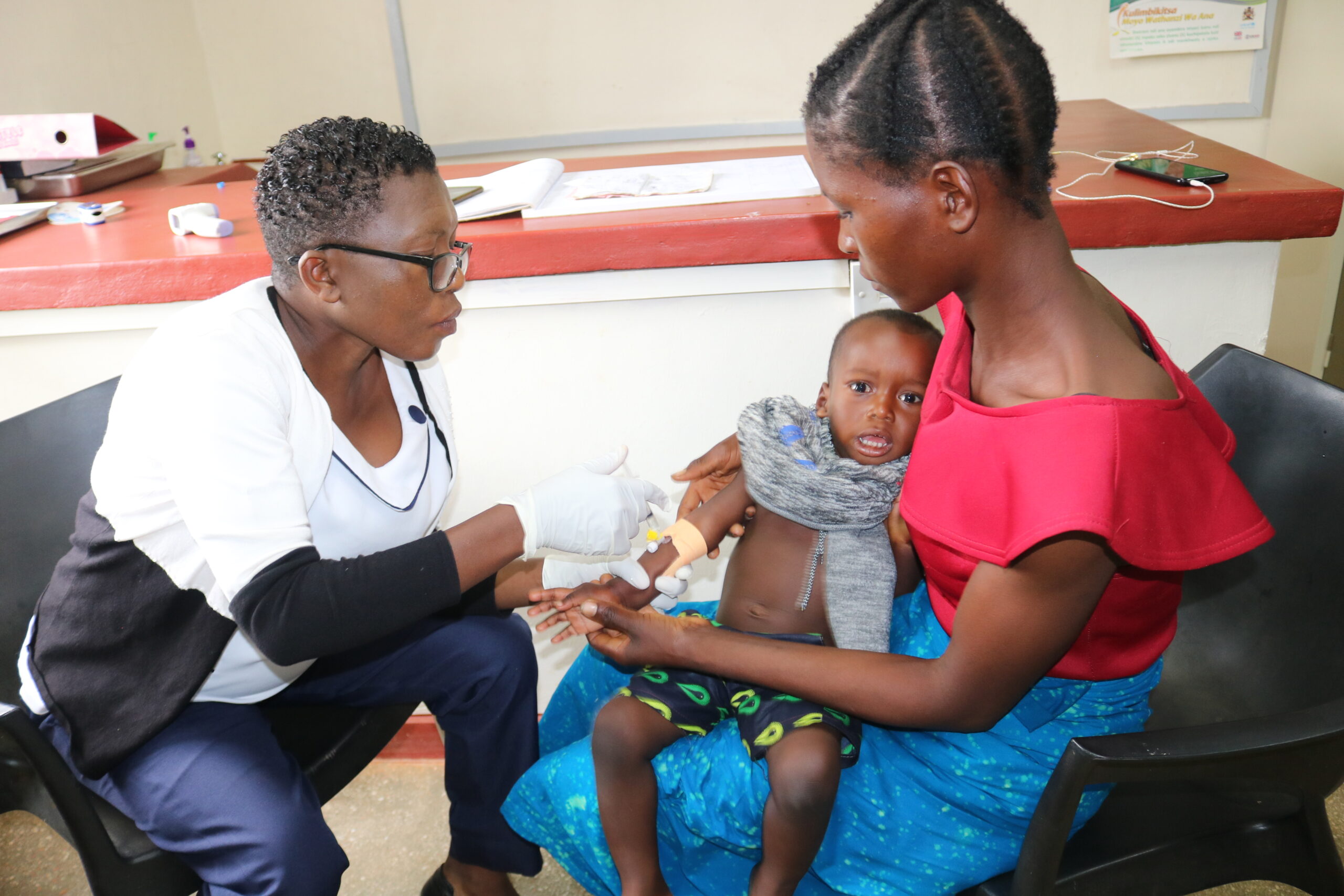
Injection Room
Thomas carries a three-year old boy into the Injection Room, a corner of the community building separated from other patients by dividersThe boy’s mother follows close behind. The child is severely dehydrated and weak. George, the lead clinician comes in and they begin preparing the IV cannula. They inject medicine and solution. In an hour or two, they will know if the child needs to be rushed to the hospital or if the injection has done its job. Malaria is treatable, but it remains deadly for children under 5, especially in rural areas.
1:00pm
Clinicians
There are two long lines leading out the door of the community building. When followed, both of the lines lead to one of two fold-out tables with a chair on one side and a seated clinician on the other. George, our Lead Outreach Clinician, and Douglas, our Support Clinician, are each busy with a patient. They listen closely and give every patient important one-on-one time before prescribing them medicine and sending them to the cashier.
By the end of the day, George and Douglas are both tired after seeing over 200 patients each.
1:30pm
Cashier
Lexa is a Patient Care Attendant, the cashier, and everyone’s favorite DJ on the long outreach clinic rides. She collects patient information, including demographics, diagnosis, and prescription. She also collects a small fee of 200MWK, equivalent to about US$0.26. These fees are directly reinvested into the medical program by paying for transport or any extra medical services for a patients’ hospital treatment. Of course, if a patient is unable to pay, they are still treated. For our records, their information is still collected.
From here, the patients go to the final stage in their journey, the pharmacy.
2:30pm
Pharmacy
The pharmacy is busy from about one hour after the start of the clinic until we are finished for the day and pack up.We would have it no other way. Our trained staff will distribute and describe prescriptions to each patient individually. Today, they will speak with over 400 patients. Upile has been working hard all day, but now she has the support of just about every Mobile Outreach Team member to make the process move quicker and smoother. It will take another hour to see the rest of the patients.

3:45pm Leaving Kambulu
After seven hours of treating patients, we’re just happy to have a trailer. We used to have to pack everything on top of the ambulance. Unpacking wasn’t too tough, but loading the crates after a long day of work was exhausting.
Now we’re back on the road headed for the Orant campus. We saw over 450 patients and tested 400 of them for malaria. In the height of the malaria season this is not unusual, especially in remote areas like Kambulu where the nearest medical center is more than 10 kilometers away and often doesn’t have medicine or even malaria test kits.
The team is a bit tired after a long day like today. Lexa puts on some mellow Malawian music and everyone relaxes. We arrive on campus at 5:40pm. We detach the trailer and Happy taxis the women to their nearby homes. Tomorrow, we will start again bright and early.